“Looking outward to the blackness of space, sprinkled with the glory of a universe of lights, I saw majesty – but no welcome. Below was a welcoming planet… That’s where life is; that’s were all the good stuff is.” – Loren Acton

Image credit: lightwise / 123RF Stock Photo
Loren Acton, an American physicist that flew into space with NASA’s Space Shuttle program in 1985, makes an excellent point that is relevant to human physiology. Earth “welcomes”, or is ideal for, our bodies because this is where we evolved to live. The human brain was designed for life on Earth, not space travel. Not to say that we should abandon exploration of this final frontier, but strange things start to happen to the body above the Earth’s atmosphere. One such anomaly is highlighted in a new study by Vignaux et al. that suggests workings of the inner ear have a say in changing the body’s bone density during space flight and potentially for aging individuals here at home on Earth.
A common misconception is that gravity does not exist in outer space, but for typical human space flight altitudes (120 – 360 miles above the Earth’s surface) this is simply not true. It does exist! The reality is that in space the gravitational force is much, much smaller than on Earth, almost zero (~ 0G).
So let’s suppose that you’re up in the space station in near zero gravity and you drop an apple out of your lunch bag. What happens? The apple appears to float, right? In actuality, the apple is falling. As a matter of fact the apple, the rest of your lunch, you, and the entire space station are falling together, not towards Earth, but around it. UPDATE (7//9/13): The condition of microgravity that is achieved through the active state of free-falling creates the experience of weightlessness. And weightlessness has been documented to wreak havoc on the human body – particularly the bones.
What happens to an astronaut’s bones in space?
Astronauts lose bone mass in space at an alarming rate. After several months on the international space station, a study found that astronauts lose 1-2% of bone mass on average per month in space, mainly in the lumbar spine and legs.
Why do astronauts lose bone density? On Earth, gravity exerts external forces on the body that challenge your bones, but in space astronauts experience prolonged weightlessness, their bones no longer bear weight, and their bodies adapt to this new environment by reducing bone mass. Basically, if you “float” everywhere and don’t need to your legs to walk around you don’t require dense bones.
The changes that occur in the space only become apparent upon returning to Earth’s gravitational forces and manifest in an increased risk of bone fracture. To counteract the musculoskeletal changes astronauts experience in space, exercise programs have been established but do not fully preserve bone mass in microgravity. Even after returning from space astronauts must go through several weeks of rehabilitation.
So how do changes in bone density occur in space, or on Earth for that matter?

Electron microscope image of an osteoclast resorbing bone. Photo credit: PathologyOutlines.com, Inc.
Bone in the body is constantly renewing itself through a maintenance procedure known as bone remodeling. Bone remodeling primarily involves two specialized types of cells: osteoclasts, bone dissolving cells, and osteoblasts, bone forming cells. In a normal healthy person, these cells strike a balance and bone is consistently being torn down and remade. In space it is thought that the working rate of the osteoclasts is increased and exceeds that of the osteoblasts, which fair less well in a microgravity environment, resulting in a bone mineral density deficit.
Bone remodeling is quite complex and several factors impact the process such as gravity, hormones, and sympathetic nervous system signaling. The sympathetic nervous system controls several of the body’s internal organs (i.e. pupil diameter, heart rate, gut mobilization) and is also involved in the body’s stress response.
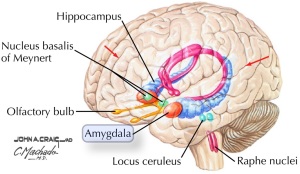
One particular component of the inner ear, the vestibular system, has been shown to alter sympathetic nerve outputs to the body. Cats with damaged vestibular nuclei, the groups of brain cells in the brainstem that receive reports from the inner ear, showed altered sympathetic nerve outputs with drops in blood pressure and increased heart rate when the animals were tilted up on a table at different angles.
So what exactly does the vestibular system do? The vestibular system acts as a sensor collecting data about the body’s position/motion and informs the brainstem, which then sends signals to various brain regions that coordinate body motion and balance. It is one of the body’s primary systems for integrating information about the force of gravity on the body. Unfortunately for the vestibular system, it was designed to function under Earth’s gravitational forces and when those are taken away in space, the system reports incorrect and disorienting information to the brain.
The big picture
Okay so let’s break down this whole scenario: The vestibular system organizes information about gravity and body position and can dictate sympathetic nerve output. In turn sympathetic nerve output has power to alter the happenings of the osteoclast-osteoblast system of bone remodeling. Vignaux et al. realized that the vestibular system is altered in the microgravity environment of space and postulated that if the vestibular system is providing the brain with incorrect information, which is what happens to astronauts in space, then incorrect sympathetic output could partially account for decreases in bone mineral density observed after extended space travel.
To test this hypothesis, Vignaux and colleagues injected rats with a chemical that damaged the inner ear, rendering it unable to sense information, mimicking how the vestibular system behaves in space. Then after a period of time they evaluated the rat’s bone mass.
A month after creating the vestibular lesions they found lower bone mineral density in the femur, the body’s largest leg bone. Numbers of osteoblasts were also reduced on the surface of the bone. Osteoclast numbers were unaffected by damaging the vestibular system. Notably, body weight as well as food and water intake were not different compared to controls suggesting that bone loss was not a result metabolic changes but rather specifically due to bone remodeling.
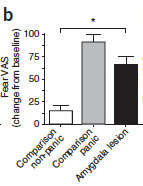
 Bone mineral density (BMD) in varying regions.
Bone mineral density (BMD) in varying regions.
The whole femur, as well as the particular portions of the femur
(distal metaphysis and disphysis regions), have significantly
lower BMD in damaged vestibular rats (VBX – gray bars)
compared to controls (Sham – white bars)
Additionally, rats were fitted with telemetric recording devices that provided information about how much or how little they moved throughout the experiment. Rats with damaged inner ears moved around twice as much as control rats with intact vestibular systems. The reason for this increase in locomotion is not well understood but it does dispel concerns that bone mineral density loss could be due to a decrease in movement and bone strain following changes to vestibular input.
To assess whether or not the changes in bone mass originated from sympathetic nervous system output to the bones, researchers used a chemical, propranolol, to block the sympathetic system output. After one month of treatment with propranolol following damage to the vestibular system, they found an increased number of osteoblast cells present on the surface of the bone and that bone loss was blunted.
What does this all mean for astronauts in space and individuals with vestibular dysfunction on Earth?
Improper vestibular signaling is an issue for astronauts living in a microgravity environment, but also for people here on Earth. Individuals with vestibular dysfunction, which can gradually occur with age, may have lower bone mineral densities which could lead to the bone loss disease known as osteoporosis. Vignaux’s results suggest that future clinical work could target the vestibular system and it’s sympathetic nervous system outputs from the brain to improve bone health. Milk! Step aside. You just aren’t getting the job done and we’re looking the inner ear for answers.
Vignaux G., Besnard S., Ndong J., Philoxène B., Denise P. & Elefteriou F. (2013). Bone remodeling is regulated by inner ear vestibular signals., Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Research, PMID: 23553797